Diagnosis of Aortic Stenosis
Aortic Stenosis can be diagnosed after detailed patient history, physical examination and echocardiography performed by specialist cardiac sonographers.
“The best thing general practitioners can do is make a habit of listening to the chest, and listening for a murmur,” explains Dr William Wilson, Interventional Cardiologist, in the below video. He further outlines the typical testing that is used to diagnose aortic stenosis, including echocardiography, ECGs, chest x-rays and blood testing.
A chest x-ray showing cardiomegaly may be indicative of left ventricular (LV) systolic failure. Other non-specific findings on a chest x-ray may be:
• calcification of the aortic valve;
• pulmonary congestion; and
• post-stenotic dilation of the aorta.
A patient with aortic stenosis may also have a systolic, ‘crescendo-decrescendo’ murmur that may be heard at the right sternal border, in the second intercostal space. This may radiate into the carotid arteries bilaterally, which is usually heard best when sitting the patient upright. The loudness of the murmur does not equate to the severity of the disease.
A 12 lead ECG at rest or during the examination may reveal evidence of Left Ventricular Hypertrophy (typically tall R waves in V5-6, and deep S wave in V1-2) in patients with Aortic Stenosis, although severe AS without significant LV Hypertrophy is a well-recognised entity.1
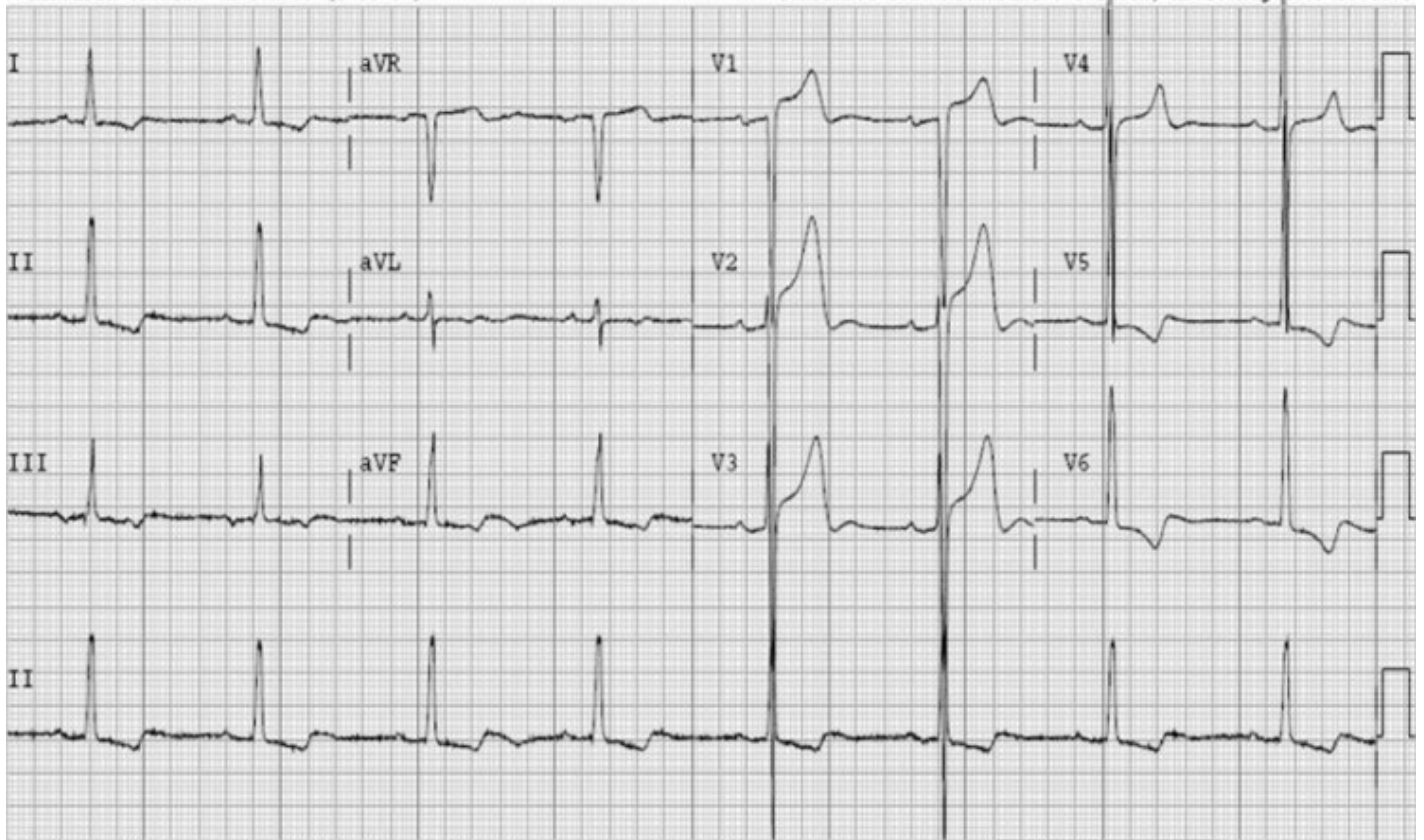
Image 1: Example of a 12 lead ECG showing left ventricular hypertrophy2
Echocardiography is one key tool for diagnosis
Patients with aortic stenosis will require complex echocardiography testing to achieve a definitive diagnosis of aortic stenosis. These specialised examinations should be performed by expertly trained cardiac sonographers who are trained in specific parameters around the diagnosis of aortic stenosis.
In the below video, Interventional Cardiologist Dr Alex Willson explains what cardiologists look for in the diagnosis of aortic stenosis, particularly on an echocardiogram. Providing a comprehensive explanation of what indications they look for during testing, he says, “once you’ve got severe aortic stenosis the leaflets are very stiff and rigid.”
The severity of aortic stenosis is determined by measuring the aortic valve area (AVA) and calculating the pressure gradient between the LV and the aorta on echocardiography. Aortic stenosis is described as mild, moderate or severe based on these measurements.
| Mean Gradient (mmHg) | Aortic Valve Area (cm2) | |
|---|---|---|
| Mild | 15-25 | >1.5 |
| Moderate | 25-40 | 1.0-1.5 |
| Severe | >40 | 0.7-1.0 |
| Critical | N/A | <0.7 |
The echocardiogram confirms the diagnosis and the severity of aortic stenosis. Two-dimensional echocardiography can demonstrate a thickened aortic valve, reduced leaflet mobility, and concentric left ventricular hypertrophy. Doppler can be used to quantify the severity of aortic stenosis by measuring the pressure gradient across the aortic valve and by calculating the aortic valve area (AVA). The velocity of blood flow across the aortic valve, as determined by continuous-wave doppler, is used to calculate the transaortic pressure gradient3.
Professor David Playford explains imaging modalities
“There does not need to be any symptoms at all to have suspicion of aortic stenosis,” Consultant cardiologist and Echocardiographic specialist Professor David Playford stresses the critical role various imaging modalities play in detecting potentially hidden aortic stenosis and diagnosing patients effectively. Learn more in the video below:
Aortic Stenosis and Heart Sounds
Interventional Cardiologist, Associate Professor Martin Ng, explains what the typical severe aortic stenosis murmur is, “described as an ejection systolic murmur… the murmur has a crescendo, it starts not as loud but becomes progressively louder, then reaches a crescendo loudness and then decreases.” He further suggests that as the condition worsens over time, the murmur will typically change.
Auscultation of the heart in patients with aortic stenosis is critical to aid in the diagnosis of the disease. As the blood is ejected from the narrowed aortic valve during systole, it is possible to hear a distinct murmur. The typical murmur of aortic stenosis is described as a high-pitched, “diamond-shaped” crescendo-decrescendo, mid-systolic murmur. The ideal location to listen to this murmur is near the right sternal border, second intercostal space. The murmur may radiate into the neck and carotid arteries.
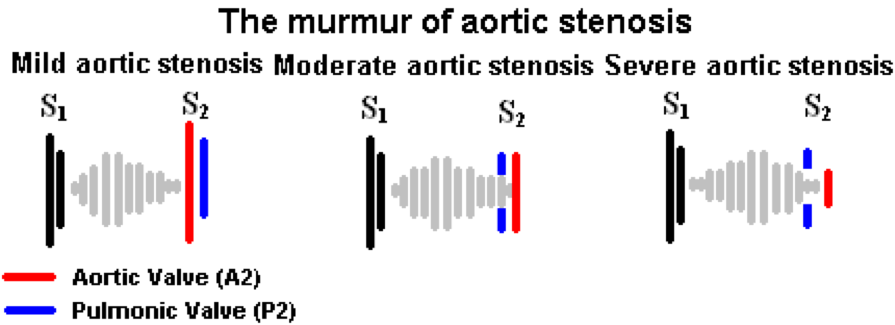
In mild aortic stenosis, the murmur peaks in early systole. However, as the disease progresses the peak moves to later in systole as a longer time is required to complete LV systole, and aortic valve closure is delayed. The intensity of the murmur typically increases as disease progresses; however, when heart failure develops and cardiac output declines, the murmur often becomes softer. Thus, the intensity of the murmur is not a good indicator of disease severity.
Listen to an Aortic Stenosis Heart Murmur
(To hear the heart sounds clearly, we recommend using your headphones)
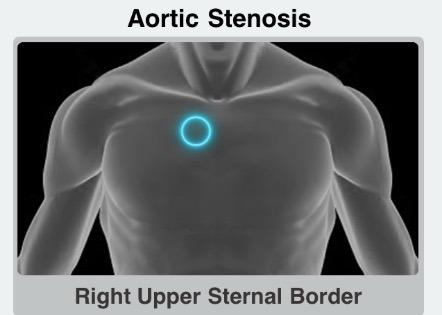
Where to Hear an Aortic Stenosis Heart Murmur
Pictured below is the ideal location to hear typical aortic stenosis murmur. Right sternal border, second intercostal space5.
Patient Disclaimer: All content on the Hope For Hearts site is created and published online for general information purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Please see your doctor if you have any questions or concerns.
- Seiler C, Jenni R. Severe aortic stenosis without left ventricular hypertrophy: prevalence, predictors, and short-term follow up after aortic valve replacement. Heart (1996); 76(3): 250-5.
- Life In The Fast Lane - ECG Library Diagnosis
- Healio - Learn The Heart
- GPOnline
- iMedicalApps
