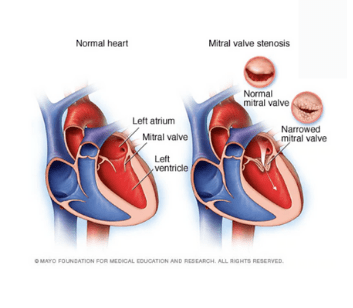
About Mitral Valve Stenosis
Mitral valve stenosis is a condition characterised by a narrowing of the mitral valve in the heart. It may reduce blood flow from the Left Atrium (LA) into the Left Ventricle (LV) affecting the amount of oxygenated blood being ejected through the LV, causing symptoms such as shortness of breath and lethargy.1
Causes of Mitral Valve Stenosis
The most common cause of mitral valve stenosis is rheumatic fever, which can damage the leaflets of the mitral valve, often caused by scarring and stretching which progressively weakens the mitral valve, and progressing to valve failure. This damage may lead to Mitral Regurgitation (backflow of blood between the left atrium and left ventricle), or an obstruction to the opening of the mitral valve which affects the amount of blood moving through the mitral valve.
Calcification of the mitral valve can also cause stenosis as a build-up of calcium deposits attach to the mitral valve which causes the valve to stiffen and reduces its ability to open/close effectively, ultimately limiting the function of the valve.
Congenital heart disease may also be responsible for mitral valve abnormalities, such as defective valve size.2
Incidence of Mitral Valve Stenosis
The actual incidence of Mitral Valve Stenosis in developed countries is relatively low, being 1 person per 100,000 people. However, rheumatic fever is the most common cause of mitral valve stenosis and is commonly found in indigenous communities in Australia. It’s estimated that indigenous Australians are 69% more likely to develop rheumatic fever and 64x more likely to develop rheumatic heart disease, which in turn affects the heart valves including the mitral valve. This disease may not be evident in the early years unless particularly severe symptoms are present and is typically discovered in the 4-5th decades of life.3
Mortality of Untreated Mitral Valve Stenosis
Untreated mitral valve stenosis has high levels of mortality in general. The mortality rates associated with untreated mitral valve stenosis are dependent on the presence of symptoms and the symptoms of pulmonary involvement/congestion. The estimated mortality rates are:
- No symptoms: survival rates > 80% survival at 10 years
- Limiting symptoms present: < 15% survival at 10 years
- Severe pulmonary hypertension: mean survival is < 3 years4
What are the signs and symptoms of Mitral Valve Stenosis?
The most common symptoms associated with mitral valve stenosis are similar to those with heart failure but may also include (but are not limited to):
- Shortness of breath (particularly when exercising),
- Heart murmur,
- Lethargy / fatigue,
- Hypertension,
- Swollen ankles,
- Cough,
- Inability to lie flat when sleeping,
- Chest pain,
- Irregular heart rate / palpitations.
Many patients with mitral valve stenosis can experience a slow progression of symptoms. For those that develop mitral valve stenosis from rheumatic fever may also not present with symptoms for many years after the disease has occurred. Due to this slow progression of the disease, it’s often associated with an unconscious, slow decline in physical activity.5
Complications of Mitral Valve Stenosis
Common complications can include:
- Atrial fibrillation (AF) is a common complication of mitral valve stenosis, due to the stretching of the left atrium which in turn can increase the incidence of atrial fibrillation
- Increased risk of thrombus formation, which can occur in patients with atrial fibrillation,
- Stroke due to thrombosis formation,
- Pulmonary hypertension,
- Infective endocarditis, and
- Heart Failure.6
How is Mitral Valve Stenosis Diagnosed?
The symptoms of mitral valve stenosis can often present as signs of heart failure, such as shortness of breath and decreased exercise tolerance. The diagnostic tests for mitral valve stenosis may include:
- Electrocardiogram (ECG): to identify irregular heart rates, such as atrial fibrillation.
- Chest x-ray: to identify an enlarged heart
- Echocardiograph (Echo): is used to measure the mitral valve and other structures within the heart to identify any abnormalities such as blood flow abnormalities. An echo can also see the pumping effectiveness of the heart which may be referred to as the “ejection fraction” (EF).
- Cardiac Catheterisation: a procedure where small catheters are introduced into the heart to identify any abnormalities of the coronary arteries which can also be responsible for symptoms. This test procedure can also be used to measure pulmonary arterial pressures to look for pulmonary hypertension which is an indication of significant mitral valve disease.7
Cardiothoracic Surgeon, Dr Andrew Newcomb discusses the diagnostic tests used to diagnose mitral valve disease in the video:
The below table outlines the currently diagnostic classifications and severity of Mitral Valve Stenosis:

Treatment Options for Mitral Valve Stenosis
Patients with mitral valve stenosis may require a combination of medical and surgical management as the condition progresses and symptoms are present. Surgical replacement of the diseased valve is the definitive treatment of mitral valve stenosis, however, this may be considered a high-risk procedure and early medical management may assist in the limitation of symptoms. Many patients with mitral valve stenosis may also have other comorbid medical conditions that can subsequently require complex medical management in conjunction with their General Practitioner, Cardiologists and Cardiac Surgeons.
Medical management of Mitral Valve Stenosis
The presence of Atrial Fibrillation (AF) in patients with mitral valve stenosis may require the administration of:
- Anticoagulants to reduce the risk of clot formation and stroke
- Medications to control AF:
- Heart rate
- Heart rhythm
- Heart Failure medications
- Diuretics
- Antihypertensives
Medical management also includes the prevention of endocarditis, which can be considered high risk in patients undergoing dental procedures involving the mucosa and gingival tissue. These patients should be considered for prophylactic antibiotic coverage.8
Procedural Management of Mitral Valve (MV) Stenosis
A mitral valve replacement may be indicated in patients with moderate to severe mitral valve stenosis. In some cases, a Mitral Valve Balloon Valvuloplasty can be considered as an interim measure to increase the size of the mitral valve. This procedure may relieve symptoms in some cases but is considered to be a temporising treatment and patients may require further intervention.
Cardiac surgery may be considered for patients whose mitral valve stenosis is so severe that the replacement of the mitral valve entirely is the most suitable therapy.
Surgical Approaches
There are two surgical techniques used to replace the mitral valve in surgery: Open Heart Surgery and Minimally Invasive Surgery
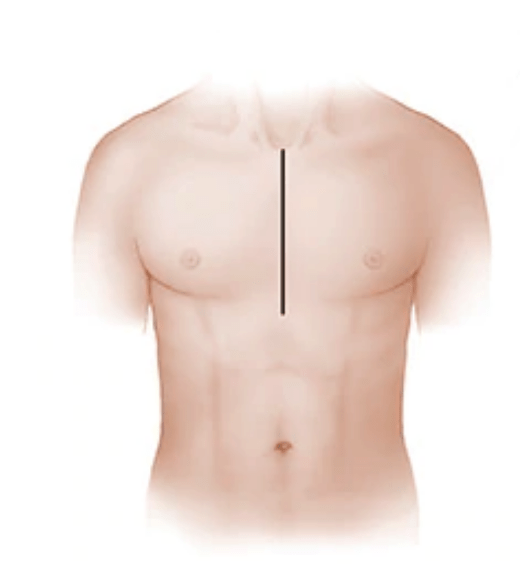
Open heart surgery requires an incision through the sternum to allow open access to the heart and structures surrounding it. The patient may or may not be put on a “heart-lung” machine which temporarily takes over the function of the heart for the duration of the procedure.
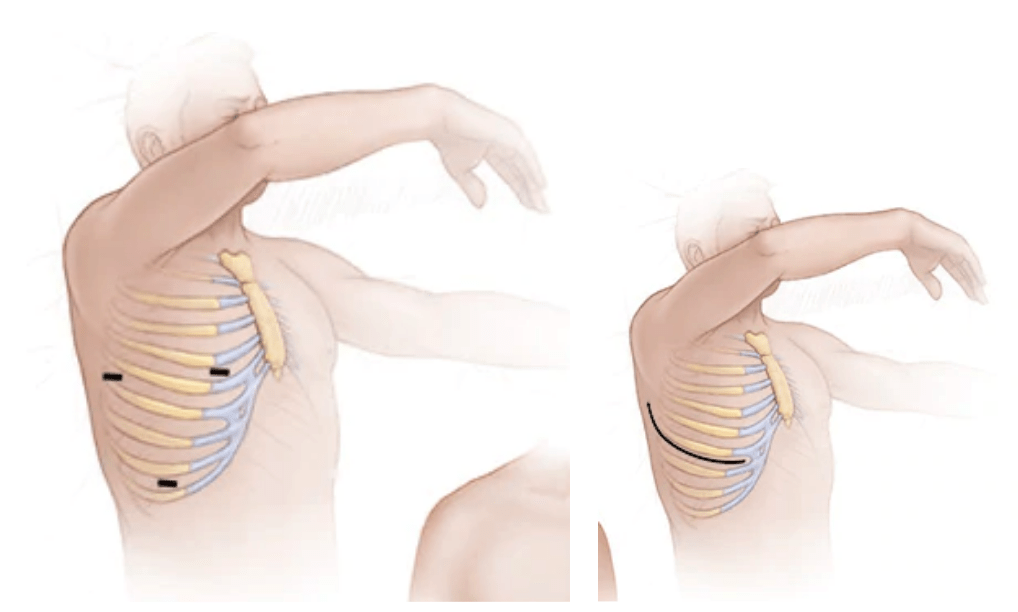
Minimally invasive surgery can use a number of areas to surgical approaches to access the diseased mitral valve and uses small incisions or “robotic” equipment to replace the mitral valve. This minimally invasive approach can result in a faster recovery and less post-operative complications, though it may not be suitable for all patients. The Cardiac Surgery team will decide what option is best for each individual.
Types of Replacement Valves
There are two distinctly different replacement valves available, tissue and mechanical valves. A cardiac surgeon will determine which valve is most suitable for each individual patient. The age at which a patient requires a valve replacement may influence the valve choice.
- Tissue Valves are either Porcine (pig) tissue of Bovine (beef) tissue. These valves are stitched onto a metal frame that is then implanted to replace the diseased valve. They have a 10-15 year life span and may then require replacement.
- Mechanical Valves are a metal component (usually cobalt) that is also attached to a metal frame and implanted. These valves may require patients to take life long anticoagulation medication due to the potential for blood clot formation. Mechanical valves will most likely last a lifetime for most patients.

“Age by itself doesn’t tell you whether someone is old or young.” Cardiothoracic Surgeon, Dr Doug Wall discusses how the age and co-morbidities of a patient determine which valve may be most suitable for them in the below video.
