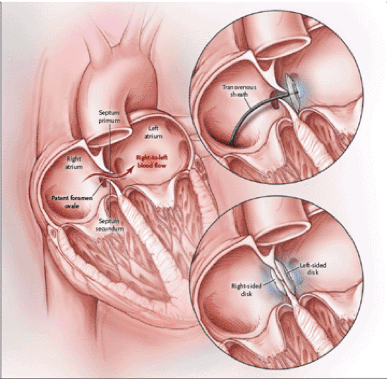
About Patent Foramen Ovale
The foramen ovale is a natural occurrence in all babies, it is a connection between the right atria (RA)and the left atria (LA) that allows foetal blood to bypass immaturely developed lungs in utero. In approx. 75 % of people it will close naturally in the first few months / years of life1.
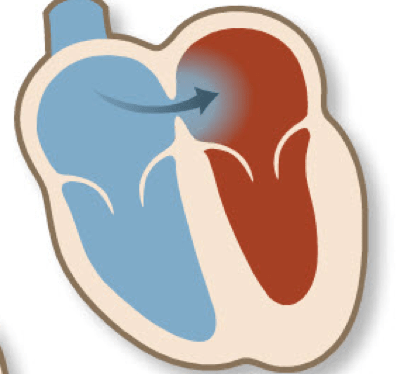
A PFO may have multiple shapes and sizes dependent on the individual and as such can be considered a simple or complex clinical structure. The predominant shunt is LA to RA, but that may be influenced by many factors such as the presence of pulmonary hypertension. The may allow small blood clots that may form in the heart to enter the lungs or the brain of patients with a PFO, causing a stroke for example. The impact clinically may also vary depending on activities that have the potential to, alter the pressure gradient within the RA/LA structures such as a Valsalva movement. The presence of a PFO may also occur alone or in the presence of other congenital defects3.
Presentation of PFO:
PFO are often undiagnosed as there are no obvious signs and symptoms or complications with an undiagnosed PFO. In adulthood, many PFO’s are found after presenting with a stroke or cerebral vascular event (CVA). These strokes with no known causes are called Cryptogenic strokes (CS). It is thought that a PFO may potentially increase the risk of a Cryptogenic stroke in some patients4.
PFO’s have also been linked to migraine headaches with aura although the mechanism of cause/ effect is not well understood. There are currently several studies looking at a causal between migraines and PFO’s5.
Diagnosis of PFO:
Echocardiography (either transthoracic or transoesophageal approach) is the predominant diagnostic tool, however, the lack of symptoms of a PFO means that many people may present as a consequence of PFO such as post cryptogenic stroke for example6.
Treatment of PFO:
Many PFO’s do not need intervention unless patients present with Cryptogenic Stroke (CS), Transient Ischaemic attack (TIA) or other congenital heart defects such as Atrial Septal Aneurysm.
Medical Treatment:
May include commencement of anti-coagulant medication after a CS or TIA, to prevent any clots from passing through the PFO.
Surgical Treatment:
Should the PFO be considered problematic, your Cardiac Surgeon or Cardiologist may suggest surgical closure of the PFO using a number of strategies dependent on the size, position and presence of other congenital heart defects7.